The Haven
Healing Centre
The Orchard
Draycott Rd, Cheddar
Somerset

The Haven |

|
| Natural Complementary Therapies - your key to improved health and well-being | |
|
Home About Contact Gift Solutions Articles Treatments Products Page: 1 2 3 4 5 Appointments |
Ankylosing Spondylitis - treat with Spinal TouchA Beneficial Treatment for Problems of Vertebral FusionAnkylosing Spondylitis treatments (using Spinal Touch Therapy) at The Haven Healing CentreAnkylosing spondylitis (AS), a form of Spondyloarthritis, is a chronic, inflammatory arthritis and autoimmune disease. It mainly affects joints in the spine and the sacroilium in the pelvis, causing eventual fusion of the spine. It has a strong genetic character. Complete fusion results in a complete rigidity of the spine, a condition known as 'bamboo spine'. Signs and symptoms Typically the patient is a young male, aged 18�30, when symptoms of the disease first appear, with chronic pain and stiffness in the lower part of the spine or sometimes the entire spine, often with pain referred to one or other buttock or the back of thigh from the sacroiliac joint. 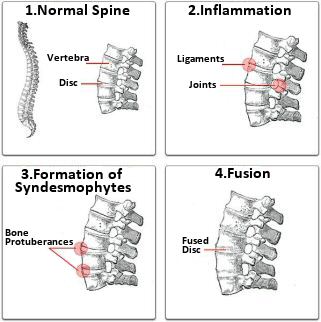 Men are affected more than women by a ratio about of 3:1, with the disease usually taking a more painful course in men than women. In 40% of cases, ankylosing spondylitis is associated with an inflammation of the eye (iridocyclitis and uveitis), causing redness, eye pain, vision loss, floaters and photophobia. Another common symptom is generalised fatigue and sometimes nausea. Less commonly aortitis, apical lung fibrosis and ectasia of the sacral nerve root sheaths may occur. As with all the sero-negative spondylo-arthropathies, lifting of the nails (onycholysis) may occur.
Men are affected more than women by a ratio about of 3:1, with the disease usually taking a more painful course in men than women. In 40% of cases, ankylosing spondylitis is associated with an inflammation of the eye (iridocyclitis and uveitis), causing redness, eye pain, vision loss, floaters and photophobia. Another common symptom is generalised fatigue and sometimes nausea. Less commonly aortitis, apical lung fibrosis and ectasia of the sacral nerve root sheaths may occur. As with all the sero-negative spondylo-arthropathies, lifting of the nails (onycholysis) may occur.When the condition presents before the age of 18, it is relatively likely to cause pain and swelling of large limb joints, particularly the knee. In pre-pubescent cases, pain and swelling may manifest in the ankles and feet, where calcaneal spurs may also develop. The spine may be affected later on. Pain is often severe on rest, and improves with physical activity, but many experience inflammation and pain to varying degrees regardless of rest and movement. Ankylosing Spondylitis is one of a cluster of conditions known as sero-negative spondylo-arthropathies, in which the characteristic pathological lesion is an inflammation of the enthesis (the insertion of tensile connective tissue into bone). Other forms of spondyloarthropathy are associated with ulcerative colitis, Crohn's disease, psoriasis, and Reiter's syndrome (reactive arthritis). Ankylosing Spondylitis is a systemic rheumatic disease meaning it affects the entire body. 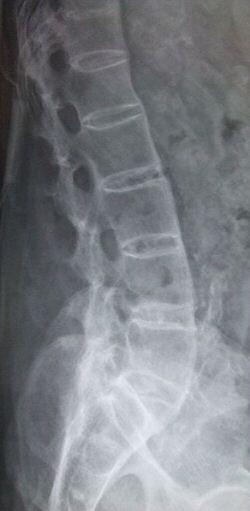 Diagnosis
DiagnosisThere is no direct test to diagnose AS. A clinical examination and X-ray studies of the spine, which show characteristic spinal changes and sacroiliitis, are the major diagnostic tools. A drawback of X-ray diagnosis is that signs and symptoms of AS have usually been established as long as 8�10 years prior to X-ray-evident changes occurring on a plain film X-ray, which means a delay of as long as 10 years before adequate therapies can be introduced. Options for earlier diagnosis are tomography and magnetic resonance imaging of the sacroiliac joints, but the reliability of these tests is still unclear. The Schober's test (a test used in rheumatology to measure the ability of a patient to flex his/her lower back) is a useful clinical measure of flexion of the lumbar spine performed during examination. During acute inflammatory periods, AS patients will sometimes show an increase in the blood concentration of C-reactive protein (CRP) and an increase in the erythrocyte sedimentation rate (ESR), but there are many with AS whos CRP and ESR rates do not increase so normal CRP and ESR results do not always correspond with the amount of inflammation a person actually has. Sometimes people with AS have normal level results, yet are experiencing a significant amount of inflammation in their bodies. Variations of the HLA-B gene increase the risk of developing ankylosing spondylitis, although it is not a diagnostic test. Over 95% of people that have been diagnosed with AS are HLA-B27 positive, although this ratio varies from population to population (only 50% of African American patients with AS possess HLA-B27, and it is close to 80% among AS patients from Mediterranean countries). In early onset disease HLA-B7/B*2705 heterozygotes exhibited the highest risk for disease. In 2007, a collaborative effort by an international team of researchers in the U.K., Australia and the United States led to the discovery of two genes, ARTS1 and IL23R, that also contribute to the cause of AS. The findings were published in the November 2007 edition of Nature Genetics, a journal that emphasizes research on the genetic basis for common and complex diseases. Together with HLA-B27, these two genes account for roughly 70 percent of the overall incidence of the disease. The Bath Ankylosing Spondylitis Disease Activity Index (BASDAI), developed in Bath (UK), is an index designed to detect the inflammatory burden of active disease. The BASDAI can help to establish a diagnosis of AS in the presence of other factors such as HLA-B27 positivity, persistent buttock pain which resolves with exercise, and X-ray or MRI evident involvement of the sacroiliac joints. The Bath Ankylosing Spondylitis Functional Index (BASFI) is a functional index which can accurately assess a patient's functional impairment due to the disease as well as improvements following therapy. The BASFI is not usually used as a diagnostic tool but rather as a tool to establish a patient's current baseline and subsequent response to therapy. Treatment No cure is known for Ankylosing Spondylitis, although treatments and medications are available to reduce symptoms and pain. Physical therapy and exercise, along with medication, are at the heart of therapy for ankylosing spondylitis. Physiotherapy and physical exercises are preceded by medical treatment in order to reduce the inflammation and pain, and are commonly followed by a physician. This way the movements will help in diminishing pain and stiffness, while exercise in an active inflammatory state would just make the pain worse. Normal occupations may be precluded by the symptoms of the disease. Some may require the help of walking aids such as a cane to help assist in balance and relieve some pressure on affected joints while walking and standing. Many with AS find it very difficult to sit or stand for prolonged periods of time which can even be about 20 minutes, therefore many need to alternate times of sitting and standing, as well as times of rest. Medical professionals and experts in Ankylosing Spondylitis have speculated that maintaining good posture can reduce the likelihood of a fused or curved spine which occurs in a significant percentage of diagnosed persons. This is where Spinal Touch can play a valuable part in your treatment plan. Spinal Touch Therapy can help to reduce symptoms, stiffness and pain in the lumbar spine and sacral areas. It is useful in relieving pressure on affected joints and therefore has a useful role in acute and palliative care. I advise anyone currently suffering with Ankylosing Spondylitis visit The Haven Healing Centre in Cheddar for a course of treatment. Appointments and a treatment price list are available by clicking here. I look forward to welcoming you soon. Phil. Medication There are three major types of medications used to treat ankylosing spondylitis. Anti-inflammatory drugs, which include NSAIDs such as ibuprofen, phenylbutazone, indomethacin, naproxen and COX-2 inhibitors, which reduce inflammation and pain. Opioid analgesics have also been proven by clinical evidence to be very effective in alleviating the type of chronic pain commonly experienced by those suffering from AS, especially in time-release formulations. DMARDs such as ciclosporin, methotrexate, sulfasalazine, and corticosteroids, used to reduce the immune system response through immunosuppression; TNFa blockers (antagonists) such as etanercept, infliximab and adalimumab (also known as biologics), are indicated for the treatment of and are effective immunosuppressants in AS as in other autoimmune diseases; TNFa blockers have been shown to be the most promising treatment, slowing the progress of AS in the majority of clinical cases, helping many patients receive a significant reduction, though not elimination, of their inflammation and pain. They have also been shown to be highly effective in treating not only the arthritis of the joints but also the spinal arthritis associated with AS. One of the many reasons sufferers are turning to complementary therapies for AS is simply because of the side effect risks to health of heavy doses of medication. But rather than looking to replace medication with physical treatment, perhaps a more sensible approach is to use physical treatment as a way of greatly cutting back on the medication. Using medications in a more restrictive way seems to make them more effective, as you don't build up the tolerance so quickly, and less becomes more in the long term. In addition, a drawback, besides the often high cost, is the fact that these drugs increase the risk of infections. For this reason, the protocol for any of the TNF-a blockers include a test for tuberculosis (like Mantoux or Heaf) before starting treatment.  In case of recurrent infections, even recurrent sore throats, the therapy may be suspended because of the involved immunosuppression. Patients taking the TNF medications are advised to limit their exposure to others who are or may be carrying a virus (such as a cold or influenza) or who may have a bacterial or fungal infection.
In case of recurrent infections, even recurrent sore throats, the therapy may be suspended because of the involved immunosuppression. Patients taking the TNF medications are advised to limit their exposure to others who are or may be carrying a virus (such as a cold or influenza) or who may have a bacterial or fungal infection.Surgery In severe cases of AS, surgery can be an option in the form of joint replacements, particularly in the knees and hips. Surgical correction is also possible for those with severe flexion deformities (severe downward curvature) of the spine, particularly in the neck, although this procedure is considered very risky. In addition, Ankylosing Spondylitis can have some manifestations which make anaesthesia more complex. Changes in the upper airway can lead to difficulties in intubating the airway, spinal and epidural anaesthesia may be difficult owing to calcification of ligaments, and a small number have aortic regurgitation. The stiffness of the thoracic ribs results in ventilation being mainly diaphragm-driven, so there may be a decrease in pulmonary function. Physical Therapy All physical therapies must be approved in advance by a rheumatologist, since movements that normally have great benefits to one's health may harm a patient with Ankylosing Spondylitis; massages and physical manipulations should only be practiced by therapists familiar with this disease. Some of the therapies that have been shown to benefit Ankylosing Spondylitis patients include:
AS can range from mild to progressively debilitating and from medically controlled to refractive. Some have times of active inflammation followed by times of remission, while others never have times of remission and have acute inflammation and pain. Unattended cases of AS that are accompanied by dactylitis or enthesitis especially when spine inflammation is not yet active, may result in a misdiagnosis of normal rheumatism. In a long-term undiagnosed period, osteopenia or osteoporosis of the AP spine may occur, causing eventual compression fractures and a back "hump". Typical signs of progressed AS are the visible formation of syndesmophytes on X-rays and abnormal bone outgrowths similar to osteophytes affecting the spine. The fusion of the vertebrae paresthesia is a complication due to the inflammation of the tissue surrounding nerves. Organs commonly affected by AS, other than the axial spine and other joints, are the heart, lungs, colon, and kidney. Other complications are aortic regurgitation, Achilles tendinitis, AV node block and amyloidosis. Owing to lung fibrosis, chest X-rays may show apical fibrosis while pulmonary function testing may reveal a restrictive lung defect. Very rare complications involve neurologic conditions such as the cauda equina syndrome. Epidemiology Three men are diagnosed with AS for every one woman; the overall prevalence is 0.25%. Many rheumatologists believe the number of women with AS is underdiagnosed, as most women tend to experience milder symptoms. History Leonard Trask, the Wonderful Invalid. It has been suggested that AS was first recognized as a disease which was different from rheumatoid arthritis by Galen as early as the second century A.D.; however, skeletal evidence of the disease (ossification of joints and entheses primarily of the axial skeleton, known as "bamboo spine") was first discovered in an archaeological dig that unearthed the skeletal remains of a 5000-year�old Egyptian mummy with evidence of "bamboo spine". The anatomist and surgeon Realdo Colombo described what could have been the disease in 1559, and the first account of pathologic changes to the skeleton possibly associated with AS was published in 1691 by Bernard Connor. In 1818, Benjamin Brodie became the first physician to document that a patient believed to have active AS had accompanying iritis. In 1858, David Tucker published a small booklet which clearly described a patient by the name of Leonard Trask who suffered from severe spinal deformity subsequent to AS. In 1833 Trask fell from a horse, exacerbating the condition and resulting in severe deformity. This account became the first documented case of AS in the United States, since its indisputable description of inflammatory disease characteristics of AS, and the hallmark of deforming injury in AS. It was not until the late nineteenth century (1893-1898), however, when the neurophysiologist Vladimir Bekhterev of Russia in 1893, Adolph Str�mpell of Germany in 1897, and Pierre Marie of France in 1898, were the first to give adequate descriptions which permitted an accurate diagnosis of AS prior to severe spinal deformity. For this reason, AS is also known as Bechterew Disease or Marie�Str�mpel Disease. Using Spinal Touch for Ankylosing Spondylitis. I hope you have found this information useful and feel encouraged to look for a solution. Please contact me if you want to find out about appointments and prices. I look forward to hearing from you. Phil. Please share this page with your friends. Thank you.
Note: DISCLAIMER: This information is not presented by a medical practitioner and is for educational and informational purposes only. The content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read. It's a small investment in yourself, but could be a life-changing experience you will cherish forever. |
| Copyright © Philip Chave 2008- TheHavenHealingCentre.co.uk All rights reserved. Email: privacy |